Article of the Week: Vocal Cord Dysfunction
In VCD, the inspiratory limb often appears flattened or coved due to paradoxical vocal fold closure during inspiration. This pattern is a key diagnostic clue that differentiates VCD from asthma, where the expiratory limb is predominantly affected.
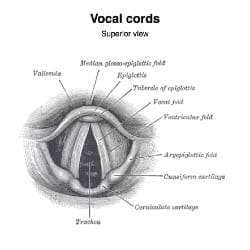
“All that wheezes is not asthma!”
Oft heard in Internal Medicine. Whose quote? 👉
This quote is widely attributed to Chevalier Jackson (of the metal Jackson tracheostomy tube fame), ENT surgeon.
He was also the father of endoscopy and supposedly retrieved over 2000 foreign bodies from his pts’ airways.
He published this quote in Boston Medical Quarterly in 1865.

Early Spiro 🧘♀️
Any idea that the origins of pulmonary function testing can be traced back to the mid-19th century?
In 1846, John Hutchinson invented the spirometer—a groundbreaking device that laid the foundation for modern respiratory diagnostics.
Thanks to him, we can now use flow-volume loops to distinguish complex airway disorders like Vocal Cord Dysfunction (VCD) from more common conditions such as asthma.
Article of the Week 📑
Diagnosis of Vocal Cord Dysfunction/ Inducible Laryngeal Obstruction: An International Delphi Consensus Study
👉 Open Source PDFThe article is open source. Feel free to read and comment your thoughts below.
VCD is basically reversible laryngeal narrowing. That’s the simple consensus definition in this article.
They used the Delphi method and specifically two rounds. Delphi is one and common way of generating expert consensus in medicine. It has limitations, like anything, but fortunately avoids groupthink and participants can be anonymous.
What I think is important about this paper is reading for awareness of VCD as a differential.
Vocal cord dysfunction is a possible diagnosis that does not get much attention in the beginning of a pt’s respiratory distress and/or workup.
But it’s very important to be included in the workup of asthma and exacerbations. It becomes important for ER, Pulmonary, Allergy, ENT, Primary care, etc. in order to understand definitions and workup as all of these specialists and physician groups may see th coughing, wheezing cohort.
Flow-Volume Loops in VCD:
Flow-volume loops graphically display the rate of airflow during inspiration and expiration.
In VCD, an abnormal flattening or truncation is typically seen on the inspiratory limb.
Why?
Well, this is due to paradoxical vocal fold motion that restricts airflow when the patient inhales.
This pattern contrasts with the expiratory limitations seen in obstructive diseases like asthma.
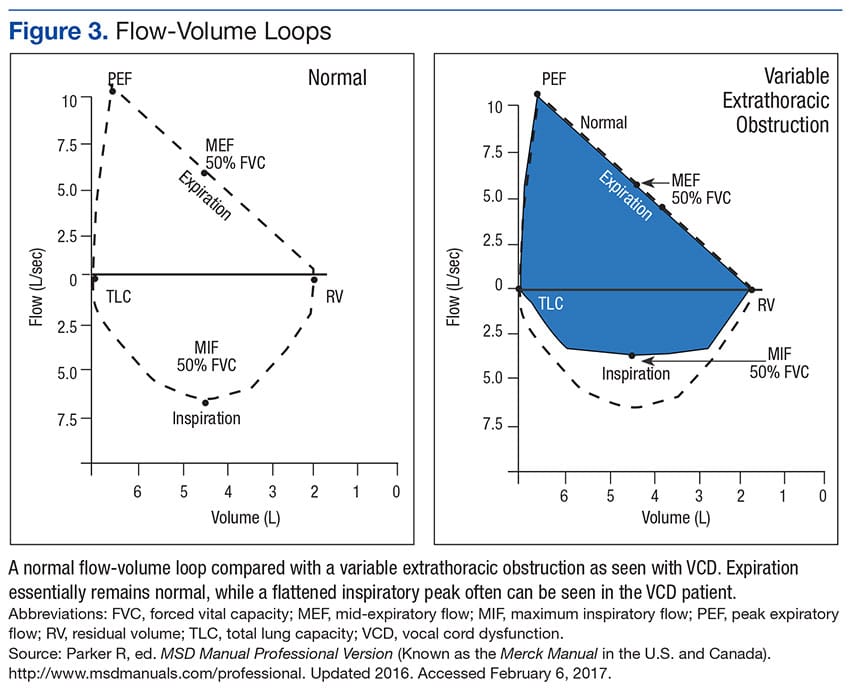
Recognizing these distinctive shapes on PFTs enables clinicians to differentiate VCD from lower airway pathologies and avoid misdiagnosis and unnecessary treatments.
Role of Amitriptyline:
Amitriptyline’s neuromodulatory properties are thought to dampen the heightened sensory responses of the larynx, thereby reducing cough frequency and intensity.
This therapeutic effect helps patients who suffer from persistent symptoms despite conventional treatments, offering a window of relief and improved quality of life.
How do FVLs help diagnose VCD? 👉
Flow-volume loops provide a visual representation of airflow during both inhalation and exhalation.
In VCD, the inspiratory limb often appears flattened or coved due to paradoxical vocal fold closure during inspiration.
This pattern is a key diagnostic clue that differentiates VCD from asthma, where the expiratory limb is predominantly affected.
Why is amitriptyline used in patients with VCD or chronic refractory cough? 👉
Although primarily an antidepressant, amitriptyline is used off-label for chronic refractory cough because it can reduce laryngeal hypersensitivity—the overactive cough reflex triggered by even minor stimuli.
By modulating neural pathways, amitriptyline helps lower the intensity of the cough response, thereby providing symptom relief in patients who do not respond adequately to standard therapies.
What makes the inspiratory limb of the flow-volume loop so critical in diagnosing VCD? 👉
The inspiratory limb reflects the patient’s ability to draw air into the lungs.
In VCD, the paradoxical closure of the vocal folds during inspiration results in a characteristic flattening or truncation of this portion of the loop.
🥼Doctor’s Order
Understanding the nuances of flow-volume loops significantly enhances our diagnostic capabilities for Vocal Cord Dysfunction (VCD) while emphasizing the importance of a multidisciplinary approach to respiratory disorders.
Historical insights continue to inform modern clinical practices, where targeted pulmonary function test interpretation combined with innovative treatments like amitriptyline has demonstrably improved patient outcomes.
As a pulmonologist, I routinely recommend ENT consultation with in-office laryngoscopy for all patients with suspected VCD to ensure comprehensive evaluation and appropriate management.

References
- Leong et al. Vocal cord dysfunction/inducible laryngeal obstruction—2022 Melbourne Roundtable Report Respiratory. 2023 May 23;28(7):615–626. doi: 10.1111/resp.14518
- Morris MJ, Christopher KL. Diagnostic criteria for the classification of vocal cord dysfunction. CHEST 2010;138(5):1213-1223.
- Sundar KM, Stark A, Morris MJ. Laryngeal Dysfunction Manifesting as Chronic Refractory Cough and Dyspnea: Laryngeal Physiology in Respiratory Health and Disease. CHEST 2024.
- Gibson PG, Vertigan AE. Management of chronic refractory cough. BMJ 2015;351:h5590.





